📋 In This Guide
- 8 persistent myths about Hallux Rigidus that athletes still believe
- What the clinical research actually shows about activity and HR
- Exercise: what helps vs. what hurts your big toe joint
- Evidence-based approaches that let you stay active with HR
Many athletes and fitness enthusiasts live with unnecessary pain or limit their training because of widespread hallux rigidus myths that simply are not true. Hallux rigidus, degenerative arthritis of the first metatarsophalangeal (MTP) joint, affects roughly 1 in 40 adults, yet it remains one of the most misunderstood foot conditions in sports medicine. In this evidence-based guide, we debunk the most damaging hallux rigidus myths and give you the facts you need to stay active, train smarter, and make better treatment decisions.
📋 Myths Debunked in This Article
- Myth: “It’s just arthritis — nothing can be done” — Grades 1–2 have excellent conservative outcomes
- Myth: “Surgery is inevitable” — Most patients never need it with proper footwear and orthotics
- Myth: “Running caused it” — Genetics and foot structure are bigger factors than activity
- Myth: “Rest is always best” — Low-impact activity and physical therapy can actually slow progression
What Is Hallux Rigidus? A Quick Refresher
Before diving into the hallux rigidus myths, here is a brief overview. Hallux rigidus is a progressive arthritic condition where cartilage in the big toe’s MTP joint wears down, causing pain, stiffness, and loss of dorsiflexion (upward bend). According to the American Orthopaedic Foot and Ankle Society, it is the most common arthritic condition of the foot. For athletes, the impact on push-off mechanics can be significant, affecting running gait, jump performance, and overall training capacity. See our full overview at what is hallux rigidus.
Myth 1: Hallux Rigidus Only Affects Older Adults
The Truth: While hallux rigidus is more common after age 30, it absolutely affects younger athletes. Research published in the Journal of Bone and Joint Surgery found that nearly one-third of patients are under 45.
High-impact sports that stress the MTP joint, such as football, soccer, gymnastics, and long-distance running, can accelerate cartilage breakdown in athletes as young as their 20s. Early recognition is key, which is why knowing the early signs of hallux rigidus matters enormously for athletes.
Myth 2: If You Can Still Walk, It Is Not Serious
The Truth: Being able to walk does not mean hallux rigidus is mild or that it should be ignored. Many athletes compensate by shifting weight to the outer foot, which creates a cascade of biomechanical problems: knee pain, hip pain, plantar fasciitis, and even lower back issues.
Grade 1 and Grade 2 hallux rigidus can severely affect athletic performance long before walking becomes painful. The time to act is before the condition progresses to Grade 3 or 4, when surgery may be the only effective option. Learn more about the importance of early detection.
Myth 3: You Should Rest Completely and Stop All Exercise
The Truth: Complete rest is rarely necessary and can actually worsen outcomes by weakening the surrounding muscles. Most sports medicine specialists recommend activity modification rather than complete cessation. Low-impact activities like cycling, swimming, and strength training that avoid toe dorsiflexion can usually continue without issue.
The key is identifying which movements aggravate symptoms and substituting alternatives. Physical therapy focusing on strengthening the intrinsic foot muscles and improving ankle mobility is often more beneficial than rest alone.
Myth 4: Hallux Rigidus Myths Say Surgery Is Always Required
The Truth: The majority of hallux rigidus cases, particularly Grades 1 and 2, respond well to conservative management. According to current clinical evidence, non-surgical treatments, including stiff-soled footwear, custom orthotics, corticosteroid injections, and physical therapy, provide substantial relief in 55 to 80% of patients.
Surgery (cheilectomy or fusion) is reserved for Grade 3 and 4 cases or those who fail conservative care after 3 to 6 months. Finding the best shoes for hallux rigidus alone can dramatically reduce pain.
Myth 5: Custom Orthotics Do Not Help Athletes
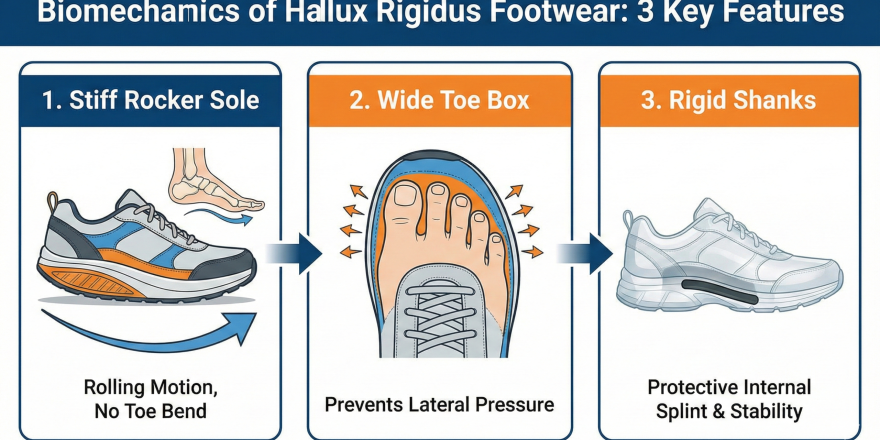
The Truth: Custom orthotics with a Morton’s extension (a rigid extension under the first metatarsal head) effectively offload the MTP joint during push-off activities. Studies show they reduce peak pressure by up to 40% at the first MTP joint. For athletes, a stiff carbon fiber plate embedded in sport-specific footwear can allow near-normal training.
Many professional athletes continue competing with hallux rigidus using the right orthotic support. See our guide on the best walking shoes for hallux rigidus for everyday options.
Myth 6: Hallux Rigidus Is the Same as a Bunion
The Truth: These are distinctly different conditions that are frequently confused, even by patients. A bunion (hallux valgus) involves lateral deviation of the big toe with a medial bony bump. Hallux rigidus causes joint stiffness and a dorsal (top) bone spur without lateral deviation.
The treatments differ significantly; bunion surgery involves realigning the toe, while hallux rigidus surgery removes bone spurs (cheilectomy) or fuses the joint. Misidentifying these conditions can lead to the wrong treatment. Our hallux rigidus diagnosis guide explains the differences in detail.
Myth 7: Pain Means the Condition Is Getting Worse
The Truth: Pain fluctuates with hallux rigidus and is not always a reliable indicator of disease progression. Many patients experience periods of significant pain followed by relative calm, regardless of whether structural changes have occurred.
Conversely, some patients with advanced Grade 3 hallux rigidus report minimal pain, particularly as motion becomes so restricted that the bone-on-bone contact stabilizes. Imaging (X-rays) is the only reliable way to assess progression. Do not let temporary pain spikes or pain relief mislead you about the actual state of your joint.
Myth 8: Young Athletes Will “Grow Out of It”
The Truth: Hallux rigidus is a degenerative condition — it does not improve on its own without treatment. While symptoms may fluctuate, the underlying cartilage damage is permanent and typically progressive. Research on the role of genetics in hallux rigidus shows that some individuals have a biological predisposition to faster progression regardless of lifestyle.
Without appropriate management, proper footwear, activity modification, and physical therapy, the condition will advance from mild (Grade 1) to severe (Grade 3-4) over time.
Myth 9: You Cannot Run or Play Sports with Hallux Rigidus
The Truth: Many competitive athletes continue training and competing successfully with hallux rigidus. The key factors are the grade of severity, sport-specific demands, and proper equipment. Runners often benefit from carbon plate shoes or custom orthotics that restrict first MTP motion.
Cyclists typically experience little to no limitation since the cycling motion does not require dorsiflexion. Swimmers are rarely affected at all. Even footballers and rugby players use sport-specific rigid-plate insoles to compete. The condition sets limits, but it does not necessarily mean the end of athletic activity.
Hallux Rigidus Myths vs. Facts: Quick Reference Table
| Myth | The Truth |
|---|---|
| Only affects older adults | Can affect athletes in their 20s and 30s |
| If you can walk, it is not serious | Compensatory gait causes widespread joint damage |
| Complete rest is required | Activity modification, not rest, is the approach |
| Surgery is always needed | 55-80% improve with conservative care |
| Orthotics do not help athletes | Carbon-plate insoles reduce MTP load by 40% |
| Same as a bunion | Completely different condition, different treatment |
| Cannot run or play sports | Many athletes compete with proper support |
| Young athletes will grow out of it | Degenerative — will not improve without treatment |
What Athletes Should Actually Do About Hallux Rigidus
Now that we have addressed the most damaging hallux rigidus myths, here is an evidence-based action plan for athletes:
- Get a proper diagnosis early. Do not wait until Grade 3 or 4. Weight-bearing X-rays confirm the grade and guide treatment.
- Choose the right footwear. Stiff-soled shoes with a rocker-bottom design minimize MTP joint stress during push-off. Check our guide on best hiking shoes for hallux rigidus if you train outdoors.
- Use custom orthotics. A Morton’s extension orthotic significantly reduces joint stress during athletic activity.
- Modify training, not eliminate it. Substitute high-impact activities with low-impact alternatives during flares.
- See a podiatrist or orthopedic surgeon if symptoms interfere with performance. Early intervention dramatically improves outcomes.
Knowing when to see a doctor for toe pain is one of the most important steps any athlete can take.
Athletes with hallux rigidus can continue training in most cases. Carbon-fibre insoles or rocker-bottom shoes reduce MTP joint stress by up to 60%. Focus on low-impact cross-training (cycling, swimming) during flare-ups and work with a sports podiatrist on footwear modifications rather than stopping activity entirely.
Frequently Asked Questions About Hallux Rigidus Myths
Can hallux rigidus get better on its own?
No. Hallux rigidus is a degenerative condition; the cartilage damage does not regenerate. Symptoms may fluctuate, but without proper treatment, the condition will progress. Early-stage disease (Grade 1) offers the most opportunity to slow progression through conservative management.
Is hallux rigidus hereditary?
Yes, genetics plays a significant role. Studies show that flat feet, elevated first metatarsal, and joint hypermobility, all genetic factors, increase the risk of developing hallux rigidus. Athletes with a family history should monitor their big toe joint health proactively.
Can I run a marathon with hallux rigidus?
Many runners complete marathons with hallux rigidus using carbon-plate shoes or custom orthotics that limit MTP joint dorsiflexion. The key is adequate preparation, appropriate footwear, and working with a sports podiatrist to protect the joint. Grade 1 and 2 cases often tolerate long-distance running well with the right support.
What sports are easiest with hallux rigidus?
Cycling and swimming are typically the most joint-friendly sports since they require little or no MTP dorsiflexion. Rowing, upper-body weight training, and yoga (seated or lying poses) are also generally well-tolerated. High-impact running, jumping, sports, and activities requiring toe push-off are most challenging.
How do I know if I have hallux rigidus or just a sprain?
A sprain typically follows a traumatic event and resolves within 4 to 6 weeks. Hallux rigidus develops gradually with progressive stiffness and pain on dorsiflexion. If your big toe pain has persisted for more than 6 weeks and you notice increasing stiffness, especially difficulty bending the toe upward, get weight-bearing X-rays rather than assuming it is a sprain.
Medically Reviewed: This article was reviewed for medical accuracy by the editorial team at HalluxRigidusCare.com. All clinical references are sourced from peer-reviewed literature and professional medical organizations.
- Hallux Rigidus Myths Debunked: What Athletes Need to Know - January 14, 2025
- What Is Hallux Rigidus? Complete Guide to Causes, Symptoms & Treatment - October 16, 2023