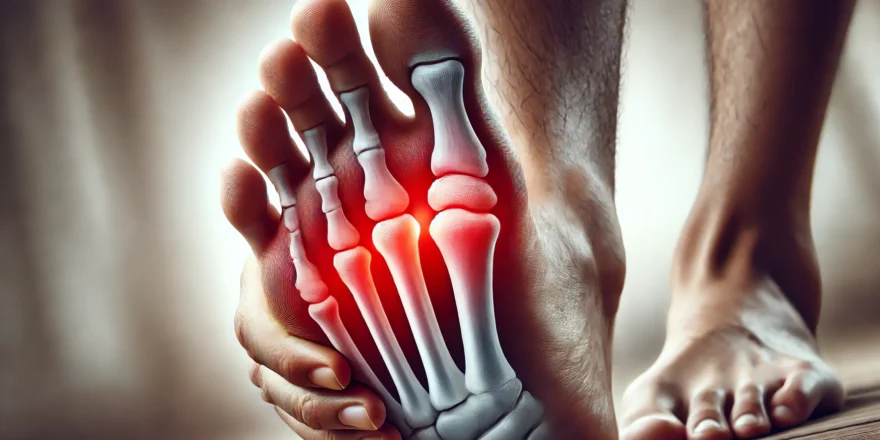
Understanding the causes of hallux rigidus is the first step toward effective management of this progressive arthritic condition. Hallux rigidus develops when cartilage in the metatarsophalangeal (MTP) joint at the base of the big toe gradually wears down, leading to bone-on-bone friction, pain, and stiffness that worsens over time without proper care.
📋 What This Guide Covers
- Root causes of hallux rigidus — from genetics to overuse injuries
- Recognisable symptoms at every stage of the condition
- Conservative treatment options include footwear, orthotics, and injections
- Surgical interventions when non-surgical care is not enough
- Recovery and rehabilitation to restore mobility after treatment
This in-depth guide covers the most common hallux rigidus causes, the symptoms that signal its presence, and the full range of treatment options — from conservative measures to surgical repair. Whether you’ve recently been diagnosed or want to understand your risk factors, you’ll find clear, evidence-based answers here.
Understanding Hallux Rigidus Causes
The big toe, medically known as the hallux, bears approximately 40% of your body weight with every step. When the MTP joint degenerates, hallux rigidus causes the toe to stiffen progressively until simple movements like climbing stairs or pushing off when running become painful.
According to the American Orthopaedic Foot & Ankle Society (AOFAS), hallux rigidus is the most common arthritic condition of the foot, affecting roughly 1 in 40 adults over age 50. Understanding the underlying causes of hallux rigidus helps patients seek timely intervention before irreversible joint damage occurs.
Causes of Hallux Rigidus

Several key factors contribute to hallux rigidus and the joint deterioration that follows. Understanding each one helps patients and clinicians determine the best preventive and treatment approach.
Genetics
Genetics can play a significant role in the development of hallux rigidus. If this condition runs in your family, you may have inherited genes that make you more susceptible. This genetic predisposition doesn’t guarantee you will develop hallux rigidus, but it does increase your risk.
Understanding your family medical history is crucial, as it can help you and your healthcare provider anticipate and monitor the condition more effectively. Learn more in our guide on hallux rigidus genetics and hereditary risk factors.
Abnormal Foot Anatomy
The way your feet are structured can also influence your likelihood of developing hallux rigidus. Certain foot types are more prone to this condition. For instance, people with a high arch or those with flat feet often experience alterations in the mechanics of their feet.
These structural anomalies place additional stress on the big toe joint, potentially leading to joint degeneration over time. Seeking appropriate footwear and orthotic support can help mitigate this risk.
Trauma
Injuries to the big toe joint, such as sprains or fractures, can be significant hallux rigidus causes. Trauma to the joint leads to premature wear and tear, disrupting its normal function and making it more vulnerable to degeneration over time. Early intervention and proper treatment after any toe injury can help minimize the long-term impact and reduce the likelihood of developing this condition.
Overuse
Repetitive stress and strain on the big toe joint can also contribute to hallux rigidus causes. This is especially common among athletes and dancers who engage in activities involving frequent and forceful foot movements, such as running, jumping, or ballet. Over time, excessive pressure on the joint leads to degeneration, resulting in pain and stiffness. Proper footwear, orthotic devices, and adequate rest are essential preventive measures for those at risk.
Arthritis
Arthritis is a significant risk factor for hallux rigidus and often serves as the primary driver of joint deterioration. Osteoarthritis, the most common type, is particularly associated with this condition.
Research published through the National Library of Medicine confirms that osteoarthritic changes are present in the majority of advanced hallux rigidus cases. Arthritis-related hallux rigidus causes are often compounded by genetics and prior joint trauma, making early arthritis management a key prevention strategy.
Symptoms of Hallux Rigidus

Hallux rigidus typically progresses gradually, with symptoms becoming more noticeable over time. Recognizing these signs early can make a significant difference in treatment outcomes. Common symptoms include:
Pain & Stiffness
The most characteristic symptom of hallux rigidus is pain and stiffness in the big toe joint. This discomfort ranges from mild to severe and often hinders your ability to move the toe freely.
The pain typically intensifies with any movement involving the big toe, walking, running, or even standing for extended periods. For a detailed overview of early warning signs, see our guide on the early signs of hallux rigidus.
Reduced Range of Motion
As hallux rigidus progresses, you’ll notice a noticeable decrease in the range of motion in your big toe. Once effortless tasks, like bending your toe or pushing off when walking, become challenging or impossible. The toe may feel rigid and unresponsive, impacting your gait and balance. Understanding the importance of early detection can help you preserve more joint function.
Hallux rigidus progresses through four distinct grades. Early diagnosis and intervention at Grades 1–2 prevents surgery in up to 90% of cases — making prompt evaluation essential when symptoms first appear.
Difficulty with Footwear
Pain and rigidity in the big toe joint make it challenging to find comfortable shoes. Tight or narrow footwear compresses the joint and worsens symptoms, while shoes with a wide toe box and stiff sole provide relief. Explore our complete guide on the best shoes for hallux rigidus to find footwear suited to your activity level and severity stage.
Hallux Rigidus Treatment Options

Treatment for hallux rigidus aims to reduce pain, improve joint function, and slow down progression. The right approach depends on the severity of the condition and the patient’s individual needs. Conservative treatments are typically the first line of defense.
Medications
Non-steroidal anti-inflammatory drugs (NSAIDs) are commonly used to manage the pain and inflammation associated with hallux rigidus. They provide short-term relief that makes daily activities more manageable and can help reduce joint swelling during flare-ups.
Orthotics
Custom orthotic devices or shoe inserts reduce pressure on the big toe joint by redistributing forces during movement. They also improve foot alignment and can play a significant role in slowing joint degeneration when used consistently.
Physical Therapy
Physical therapy involves targeted exercises and stretches to enhance joint mobility and strengthen surrounding muscles. Skilled physical therapists provide guidance on performing these exercises correctly, leading to improved function and reduced pain over time.
Footwear Modifications
Shoes with a wide toe box and a lower heel alleviate pressure on the big toe joint, allowing for more space and reduced friction. Properly fitting shoes can significantly improve the quality of life for individuals managing this condition.
Activity Modification
Avoiding or reducing high-impact sports or activities that worsen symptoms is a practical and effective strategy. Making mindful choices about physical activity can prevent further joint damage and reduce the frequency and intensity of pain episodes.
Recovery & Rehabilitation

Recovery and rehabilitation following hallux rigidus treatment vary depending on the chosen approach and the individual patient’s condition and goals.
Non-Surgical Treatment
Non-surgical treatments such as orthotics, physical therapy, and medications focus on managing pain, increasing joint mobility, and improving overall foot function. Recovery involves gradual symptom improvement over weeks to months. Consistently following your healthcare provider’s recommendations is essential for the best results.
Surgical Treatment
If non-surgical interventions fail to provide adequate relief or if hallux rigidus has progressed significantly, surgery may be necessary. Recovery following surgical procedures involves a more extended healing period — often requiring a cast, specialized footwear, and post-surgical physical therapy to restore function.
Long-Term Care
Hallux rigidus is a chronic condition requiring ongoing management to maintain foot health and quality of life. Regular follow-up appointments allow your healthcare provider to monitor progress and adjust your treatment plan as needed. If you’re unsure whether your symptoms warrant a professional evaluation, our guide on when to see a doctor for toe pain can help you decide.
Frequently Asked Questions About Hallux Rigidus Causes
What are the most common hallux rigidus causes?
The most common hallux rigidus causes include osteoarthritis, genetics, abnormal foot anatomy (flat feet or high arches), trauma to the big toe joint, and repetitive overuse through high-impact activities. In many cases, multiple factors combine to trigger or accelerate the condition.
Is hallux rigidus hereditary?
Yes, genetics is one of the recognized hallux rigidus causes. If a parent or sibling has the condition, your risk is elevated. However, lifestyle factors — including footwear choices, activity level, and weight management — can influence whether and when the condition develops.
Can hallux rigidus be prevented?
While you cannot change your genetics or natural foot structure, understanding your hallux rigidus causes can guide preventive steps: wearing supportive footwear, avoiding repetitive joint trauma, maintaining a healthy weight, and treating arthritis early can all help delay or limit the condition’s progression.
When should I see a doctor about hallux rigidus?
If you experience persistent big toe pain, stiffness, or swelling that interferes with daily activities, consult a podiatrist or orthopedic surgeon. Imaging studies such as X-rays can confirm the diagnosis and stage the condition — learn more about the role of X-rays and MRIs in detecting hallux rigidus.
Medically reviewed for accuracy. For personalized diagnosis and treatment recommendations, consult a board-certified podiatrist or orthopedic foot and ankle specialist.