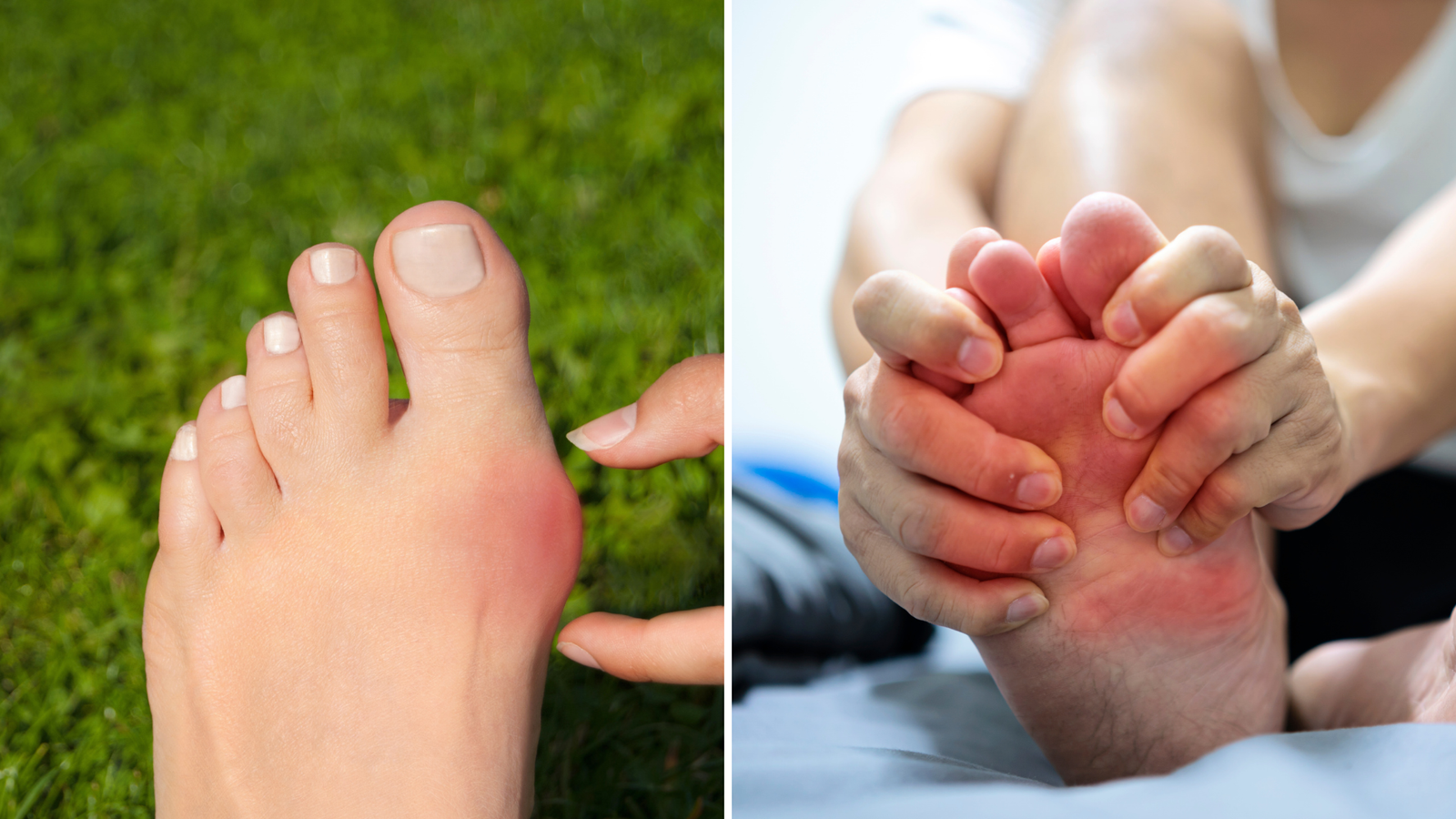
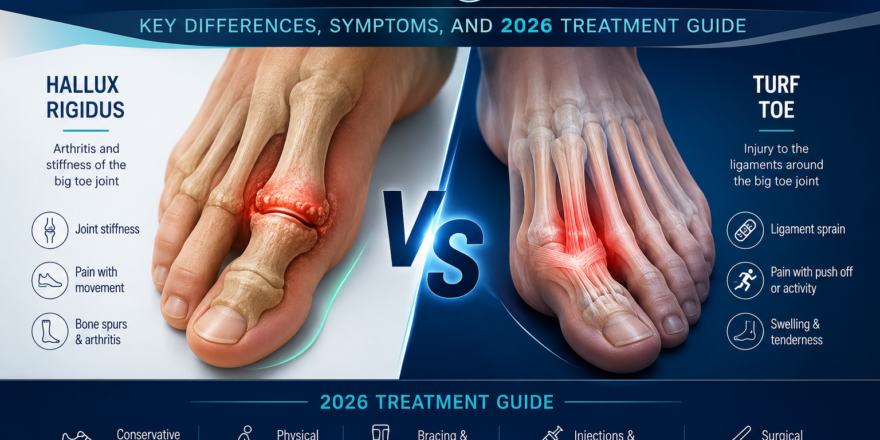
If you woke up today with a throbbing, painful big toe, you are likely asking one urgent question: Is this a gout flare or the onset of hallux rigidus?
While both conditions target the first metatarsophalangeal (MTP) joint, the “why” and “how” of the pain are opposites. In my clinical experience, misdiagnosing a metabolic fire for a mechanical grind is the leading cause of prolonged suffering and ineffective treatment.
Getting the diagnosis right is critical because the 2026 treatment protocols. It ranges from urate-lowering therapies to supercritical foam offloading, requiring precision to protect your long-term mobility. Let’s look at the pathology behind the pain.
The Mechanical Grind: Understanding Hallux Rigidus
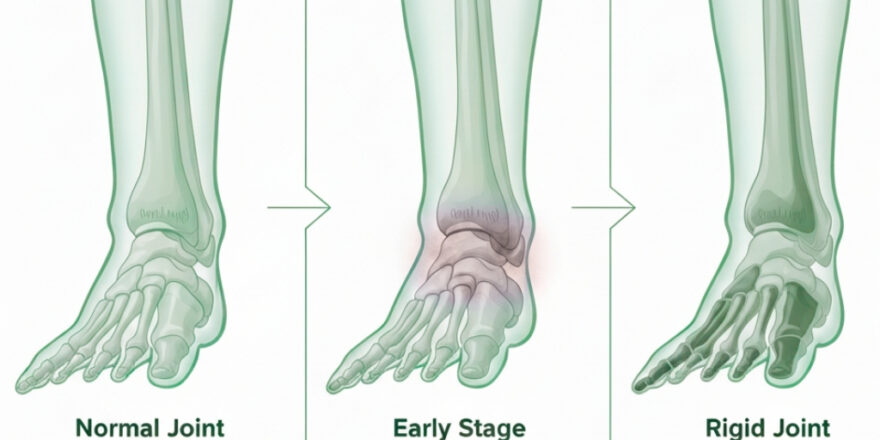
Hallux rigidus is a specific, progressive form of degenerative arthritis localized to the first metatarsophalangeal (MTP) joint. To understand this condition, you must visualize the joint as a biological hinge. In a healthy foot, this hinge is coated with smooth articular cartilage, allowing your big toe to dorsiflex (bend upward) between 65° and 90° during a normal walking stride.
When you develop hallux rigidus, the smooth, “lubricated” surface begins to break down. As the cartilage thins, the joint space narrows, leading to bone-on-bone friction. In response to this mechanical stress, your body attempts to stabilize the joint by growing new bone. These are the dorsal osteophytes, or bone spurs, that create the characteristic “hard bump” on top of your toe.
In my clinical practice, I categorize this as a structural failure. The pain is triggered by the “push-off” phase of your gait. Because bone spurs physically block the joint, every step you take in a flexible shoe forces the joint to jam against itself. Over time, this leads to subchondral sclerosis (thickening of the bone under the cartilage) and a permanent loss of motion. By 2026 standards, we no longer just look at static X-rays; we use Weight-Bearing CT (WBCT) to analyze how your body weight of 40-60% crushing down on that MTP joint during movement is accelerating this “grind.”
The 2026 Clinical Markers of Hallux Rigidus
- Crepitus: That audible or tactile “gritting” sensation when you move the toe manually.
- Functional Hallux Limitus: A stage where the toe moves fine while sitting, but “locks up” the moment you stand and put weight on it.
- Compensatory Gait: You might find yourself walking on the outside of your foot (supination) to avoid bending the painful big toe.
The Hallux Rigidus vs. Gout Diagnostic Matrix: Side-by-Side Comparison
When you are sitting on the edge of your bed, staring at a swollen big toe, you need a clear “if/then” roadmap. In 2026, we utilize a Differential Diagnosis approach that weighs metabolic markers against mechanical triggers. While both conditions cause significant distress, the “signature” of the pain is remarkably different when scrutinized under clinical light.
1. Onset and “Pain Signature”
The most telling differentiator is the speed of onset.
- Gout: This is a “Zero-to-Sixty” condition. I often hear patients describe going to bed feeling perfectly fine, only to be awoken at 3:00 AM by a pain so intense they suspect a fracture. The inflammatory cascade of monosodium urate crystals peaks rapidly, usually within 12–24 hours.
- Hallux Rigidus: This is a “Slow Burn.” It follows a predictable, degenerative curve. The pain starts as a dull ache after a long walk or a day in flexible sneakers. Over months or years, the “good days” become fewer as joint space narrowing progresses. It is a chronic “grind” rather than an episodic “flare.”
2. Visual and Thermal Presentation
If you look at your toe right now, what do you see?
- Gout: The joint will look erythematous (intensely red) and edematous (swollen). The skin often appears shiny or stretched because the inflammation is so localized and aggressive. If you place the back of your hand near the joint, it will radiate noticeable heat. In 2026, we call this the “Hot Dog” sign; the toe is red, swollen, and looks ready to burst.
- Hallux Rigidus: The toe rarely looks “angry” or red. Instead, you will see a structural change: the dorsal osteophyte. This is a hard, bony protrusion on the top of the MTP joint. It doesn’t feel like a fluid-filled cyst; it feels like an extension of the bone itself. While there may be mild swelling after activity, it lacks the systemic “heat” of a metabolic flare.
3. The “Bed Sheet Test” (Allodynia)
In my clinic, I use a simple litmus test for gout: Allodynia. This is a clinical term for pain caused by a stimulus that does not normally provoke pain.
- Gout: If the weight of a standard cotton bed sheet touching your toe feels like a hot iron, you are almost certainly dealing with a gout flare. The nerves in a gout-affected joint are hyper-sensitized by the inflammatory response.
- Hallux Rigidus: You can wear a heavy sock, touch the joint, or wrap it in a blanket without significant discomfort. The pain in Hallux Rigidus is deep and structural; it requires pressure or movement (dorsiflexion) to trigger.
4. Mechanical Triggers vs. Metabolic Triggers
What were you doing 24 hours before the pain started?
- Gout Triggers: Did you have a high-purine meal, a few beers, or perhaps a sudden bout of dehydration? In 2026, we also look closely at high-fructose corn syrup intake, which has become a primary driver of uric acid spikes in younger patients.
- Hallux Rigidus Triggers: Did you go for a run in “minimalist” or flexible shoes? Did you spend the day on a ladder or kneeling? Hallux Rigidus pain is triggered by the “push-off” phase of gait. When you try to bend a toe that is blocked by bone spurs, the joint “jams,” causing a sharp, stabbing pain at the terminal stance of your walk.
| Feature | Hallux Rigidus (Mechanical) | Gout (Metabolic) |
|---|---|---|
| Primary Cause | Cartilage wear / Bone spurs | Uric acid crystal buildup |
| Onset Speed | Gradual (Years/Months) | Explosive (Hours) |
| Skin Color | Normal or slightly pale | Fire-truck red / Purple |
| Skin Texture | Normal | Shiny / Stretched / Tight |
| Morning Sensation | Stiff, but “warms up” | Intense, throbbing pain |
| The “Grind” | Common (Crepitus) | Rare (unless chronic) |
| Home Test | Painful when pulling toe up | Painful when skin is touched |
5. Imaging: Beyond the X-Ray
In 2026, the way we “prove” these differences has evolved.
- For Hallux Rigidus: We utilize Weight-Bearing CT (WBCT). Standard X-rays taken while sitting down are deceptive because they don’t show how the joint space collapses under your actual body weight. WBCT allows Dr. Sarah to see exactly where the subchondral sclerosis is most severe.
- For Gout: We use Dual-Energy CT (DECT). This is a game-changer for 2026. DECT can differentiate between bone, calcium, and uric acid. On the screen, I can see green-colored urate deposits (tophi) hiding behind the joint. Providing a “smoking gun” for gout, even if your blood uric acid levels currently look normal (which happens in 30% of acute flares).
6. The “Range of Motion” Nuance
Finally, we look at the MTP joint dorsiflexion.
- In Hallux Rigidus, the range of motion is physically blocked. No matter how much you try, the toe will not bend upward beyond a certain point because bone is hitting bone. This is Functional Hallux Limitus.
- In Gout, the range of motion is limited by pain, not by a physical block. Between flares, a gout patient often has a perfectly normal, fluid range of motion. Something a Hallux Rigidus patient will never regain without intervention.
By using this matrix, we can move away from “guessing” and toward a precision-based treatment plan. Whether we are cooling a metabolic fire or offloading a mechanical grind, the first step is knowing exactly which “beast” we are fighting.
2026 Treatment Protocols: Cooling the Fire and Offloading the Grind
Once the diagnostic fog has cleared, the path to recovery splits into two distinct clinical lanes. Treating a structural joint (Hallux Rigidus) with metabolic medication is as ineffective as trying to “walk off” a systemic gout flare. In 2026, Dr. Sarah Jenkins’ protocol emphasizes a “Dual-Track” approach: biochemical stability for gout and biomechanical offloading for hallux rigidus.
Phase 1: Cooling the Inflammatory Fire (Gout)
For gout, the goal is to lower serum uric acid below the saturation point of 6.0 mg/dL.
- Acute Relief: We utilize a combination of Colchicine and fast-acting NSAIDs. In 2026, we prioritize starting Urate-Lowering Therapy (ULT). Such as Allopurinol, during the flare to accelerate the dissolution of crystals, a shift from older “wait-and-see” models.
- The Metabolic Reset: Dietary modification remains a cornerstone. We now focus heavily on eliminating high-fructose corn syrup and alcohol, which trigger the liver to overproduce uric acid, while encouraging low-fat dairy and Vitamin C to aid in renal excretion.
Phase 2: Offloading the Mechanical Grind (Hallux Rigidus)
Because Hallux Rigidus is a structural failure, the solution must be mechanical. We cannot “cure” a bone spur, but we can bypass it.
- The Power of Rocker Geometry: The 2026 gold standard for non-surgical relief is the Rocker Bottom Shoe. By utilizing a curved sole, the shoe handles the “push-off” for you, preventing the MTP joint from dorsiflexing into the painful bone spur.
- Supercritical Foam Technology: Modern foams, such as those found in the HOKA Bondi 9, provide a level of shock absorption that traditional orthotics cannot match. These nitrogen-infused midsoles dissipate 40-60% of body weight that normally crushes the arthritic joint during gait.
The 2026 Footwear Prescription
If you are struggling with the daily “grind” of a stiff big toe or recovering from the lingering sensitivity of a gout flare, your footwear choice is your most important daily “medication.”
- For Maximum Offloading: The HOKA Bondi 9 remains the elite choice. Its aggressive late-stage meta-rocker is specifically engineered to bypass the MTP joint entirely. You can find my full analysis in our guide to the Best Women’s Shoes for Hallux Rigidus.
- For Active Recovery: The New Balance 1080 v14 utilizes Bio-Based Fresh Foam X, offering a more flexible yet supportive transition for those in the earlier stages (Grade 1-2) of joint wear. I recommend these for men who need a transition from clinical stiffness to everyday comfort; see our Best Men’s Shoes for Hallux Rigidus for more details.
Conclusion: Taking the First Step Toward Joint Longevity
Distinguishing between Hallux Rigidus vs. Gout is a matter of preserving your ability to walk, run, and remain active. As we have explored in this 2026 guide, one condition is a metabolic fire that requires biochemical intervention, while the other is a mechanical failure that requires structural offloading.
In my years as an orthopedic specialist, I have seen far too many patients allow “the grind” to become permanent because they treated it as a temporary “flare.” If you are experiencing the deep, predictable ache of Hallux Rigidus, the most impactful change you can make today is switching to a supercritical foam rocker like the HOKA Bondi 9 or the NB 1080 v14. These shoes act as a mechanical bypass, protecting your MTP joint from further wear.
However, if your joint is red, hot, and explosive in its pain, do not wait. Seek a Dual-Energy CT (DECT) scan and consult with a rheumatologist to stabilize your uric acid levels.
Your gait is the foundation of your health. Whether you are cooling a fire or bypassing a grind, the right diagnosis is the only way to keep that foundation solid.
Frequently Asked Questions: Hallux Rigidus vs. Gout
How can I tell if my big toe pain is gout or hallux rigidus at home?
The most reliable home indicator is the “Bed Sheet Test.” If the skin on your big toe joint is so sensitive that even a light bed sheet or a sock causes excruciating pain (allodynia), it is likely Gout. If you can touch the joint and wear socks without pain, but feel a deep, sharp “grinding” ache specifically when you bend your toe upward to walk, it is almost certainly Hallux Rigidus.
Can you have both gout and hallux rigidus at the same time?
Yes. In clinical practice, this is a common “Double Threat.” Chronic gout causes the deposition of urate crystals that act like sandpaper, physically shredding the articular cartilage over time. This metabolic damage accelerates structural degeneration, often leading to a secondary diagnosis of Hallux Rigidus. If you have a known stiff big toe and suddenly experience intense redness, heat, and a spike in pain, you may be experiencing a “superimposed” gout flare.
Does hallux rigidus feel hot to the touch like gout?
No. While hallux rigidus can cause mild swelling after a long day of activity, it rarely produces the intense, radiating heat associated with a gout flare. A gout-affected joint will feel significantly warmer than the surrounding skin—a sign of a systemic inflammatory response. Hallux rigidus is a mechanical issue; the joint stays relatively cool unless there is an extreme, acute aggravation of the bone spurs.
Is the “bone bump” on my toe a gout tophi or a hallux rigidus spur?
A hallux rigidus bone spur (dorsal osteophyte) is a hard, immovable protrusion that feels like a permanent part of the bone. It is typically located on the top of the joint. A gout tophus is a collection of urate crystals; it may feel firm, but it often has a slightly “doughy” or asymmetrical texture and may appear white or yellowish under the skin. A Weight-Bearing CT (WBCT) scan is the most effective way to distinguish these structural differences.
What foods should I avoid for gout that won’t help hallux rigidus?
For gout, you must limit high-purine intake—specifically red meat, organ meats, shellfish, and beer. However, the 2026 clinical focus is on high-fructose corn syrup, which aggressively spikes uric acid levels. These dietary changes are essential for managing the “metabolic fire” of gout but will have no mechanical effect on the “grind” of hallux rigidus, which requires footwear modifications like rocker bottoms.
Why does big toe pain often peak at night?
For gout patients, pain peaks at night because core body temperature drops and your joints become slightly more dehydrated during sleep. This causes uric acid to “crash out” of the fluid and form sharp crystals. For hallux rigidus patients, “night pain” is usually an inflammatory throb following a day of overactivity or wearing unsupportive, flexible shoes that jammed the joint.
Can walking in the wrong shoes trigger a gout attack?
While shoes don’t cause the metabolic spike of uric acid, mechanical trauma to a joint can trigger a flare in people with asymptomatic hyperuricemia. If you have Hallux Rigidus and wear flexible shoes that constantly “jam” the joint. It can provide the perfect site for urate crystals to precipitate, turning a mechanical ache into a full-blown gout attack.
Is exercise good for a stiff big toe, or will it make it worse?
For Hallux Rigidus, exercise is a double-edged sword. Low-impact activities like swimming or cycling are excellent. However, running or high-impact sports can accelerate cartilage wear unless you use mechanical offloading. For Gout, you should strictly avoid exercise during an active flare, as movement can further irritate the crystal-filled joint space.
Will a cortisone shot fix hallux rigidus like it does a gout flare?
Cortisone is highly effective at “putting out the fire” of a gout flare or acute inflammation in the joint. However, in Hallux Rigidus, it is a temporary bandage. It does not remove the bone spurs or regrow cartilage. While it provides short-term relief, the mechanical “grind” will return as soon as the steroid wears off unless the structural issues are addressed.
Does hallux rigidus always require surgery?
No. Many patients manage Hallux Rigidus for decades through conservative 2026 protocols: Supercritical foam footwear, custom carbon-fiber orthotics, and activity modification. Surgery is typically only considered when the “grind” becomes so severe that it prevents daily activities even with optimized footwear like the HOKA Bondi 9.