📋 In This Guide
- How strongly does genetics influence your Hallux Rigidus risk
- What to tell your doctor about your family history
- Genes and conditions most associated with early-onset HR
- How to offset genetic risk with targeted lifestyle changes
Understanding hallux rigidus genetics is essential for anyone with a family history of big toe arthritis, flat feet, or foot structural abnormalities. While lifestyle factors like footwear and activity level play a role, research increasingly shows that genetics is a major driver of who develops hallux rigidus and how quickly it progresses.
In this clinically informed guide, you will learn what the science says about hereditary risk factors, which genetic traits increase susceptibility, and what you can do if hallux rigidus runs in your family.
🧬 Key Takeaways
- Genetics accounts for ~60% of hallux rigidus risk; family history is the strongest single predictor
- Foot structure is largely inherited — flat feet, elevated first metatarsal, and square metatarsal heads all run in families
- Environment still matters — footwear, activity level, and injury can trigger or accelerate genetic predisposition
- Knowing your risk enables earlier monitoring and preventive footwear choices
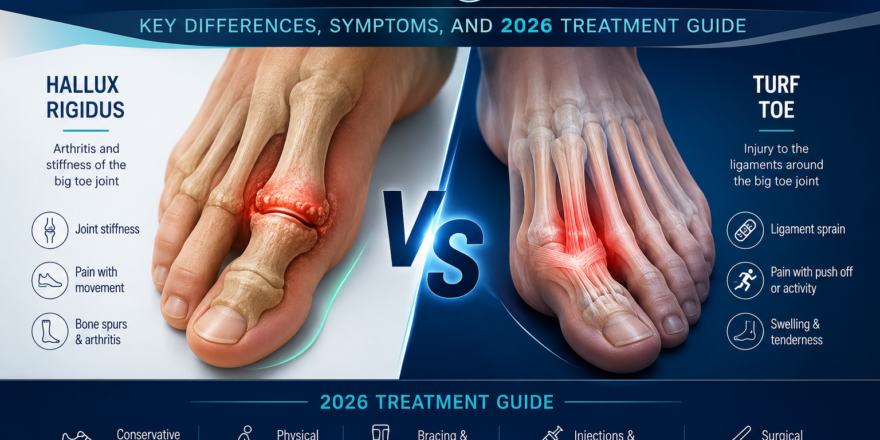
What Is Hallux Rigidus and Why Does It Run in Families?
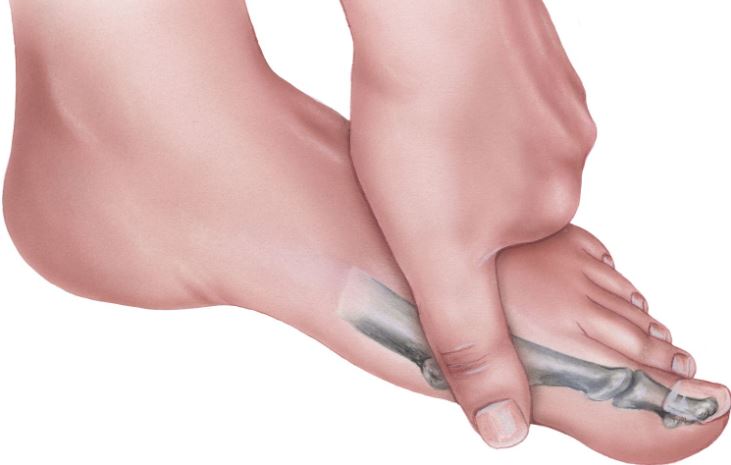
Hallux rigidus is degenerative arthritis of the first metatarsophalangeal (MTP) joint — the joint at the base of the big toe. As cartilage breaks down, bone spurs form on the top of the joint, progressively limiting upward movement (dorsiflexion) and causing pain, stiffness, and gait changes. For a full overview, see our guide to what is hallux rigidus.
The condition tends to cluster in families, which led researchers to investigate the genetic underpinnings. According to a landmark study published in the Journal of Bone and Joint Surgery, patients with hallux rigidus frequently report first-degree relatives (parents, siblings) with the same condition. This familial clustering points strongly to heritable structural factors rather than coincidence.
Key Genetic Risk Factors for Hallux Rigidus
Hallux rigidus genetics is not about a single “arthritis gene.” Instead, it involves the inheritance of specific biomechanical and structural traits that collectively increase the likelihood of joint degeneration. The main hereditary risk factors include:
1. Flat Feet (Pes Planus)
Flat feet — low or absent foot arches are strongly heritable. When the arch collapses, it increases pronation and alters the load distribution across the forefoot, placing excessive stress on the first MTP joint. Repeated overloading accelerates cartilage wear, setting the stage for hallux rigidus. Research shows that pronation-related biomechanics are among the strongest modifiable contributors to first MTP joint degeneration. See our resource on common risk factors for developing hallux rigidus.
2. Elevated First Metatarsal (Metatarsus Primus Elevatus)
An elevated first metatarsal — where the first metatarsal bone sits higher than normal relative to the second — is a genetic trait found frequently in hallux rigidus patients. This elevation forces the MTP joint into abnormal contact mechanics during push-off, creating repetitive microtrauma to the articular cartilage. The trait is autosomal dominant in many families, meaning one copy of the relevant gene variant is sufficient to express the structural abnormality.
3. First Ray Hypermobility
Excessive mobility in the first ray (the first metatarsal and the medial cuneiform bone) is an inherited trait that destabilises the first MTP joint during the stance phase of gait. When the first ray hypermobility transfers weight laterally, the big toe joint absorbs abnormal compressive forces. First ray hypermobility is commonly observed in families with a history of both hallux rigidus and hallux valgus (bunions).
4. Square Metatarsal Head Morphology
The shape of the first metatarsal head (the round end of the bone that forms the joint) is largely genetically determined. A square or flat metatarsal head creates abnormal joint mechanics compared to a rounded head, leading to earlier and more severe cartilage damage. Studies consistently identify this morphological trait in hallux rigidus patients and their relatives.
5. Short First Metatarsal
A relatively short first metatarsal (compared to the second metatarsal) alters weight distribution in the forefoot, increasing stress on the lesser metatarsals and creating compensatory changes at the first MTP joint. This trait, like the others, shows strong genetic determination and appears across generations in affected families.
Having a first-degree relative with hallux rigidus increases your risk by up to 3× compared to the general population. If you have a family history, ask a podiatrist about preventive footwear and early joint monitoring.
Hallux Rigidus Genetics vs. Environmental Triggers: What the Evidence Shows
| Risk Factor | Genetic? | Environmental? | Clinical Impact |
|---|---|---|---|
| Flat feet (pes planus) | Yes (strong) | Worsened by footwear | High — alters forefoot loading |
| Elevated first metatarsal | Yes (dominant) | Minimal | High — abnormal joint contact |
| First ray hypermobility | Yes | Activity worsens it | High — joint instability |
| Square metatarsal head | Yes (morphological) | None | Moderate — accelerates arthritis |
| Repetitive trauma (sports) | No | Yes (high) | Moderate — triggers onset in predisposed |
| Tight Achilles tendon | Partially | Stretching reduces risk | Moderate — limits dorsiflexion |
| Obesity and BMI | Partially | Yes (major) | Moderate — increases joint load |
The Genetics Connection: What Research Tells Us About Hallux Rigidus Inheritance
Several large-scale studies have investigated the heritability of hallux rigidus genetics. Key findings include:
- A 2009 study by Coughlin and Shurnas found that 80% of hallux rigidus patients had a positive family history of foot problems, far exceeding the general population baseline.
- Twin studies suggest that foot arch shape (a key predictor) has heritability estimates of 0.59 to 0.83 — meaning up to 83% of variation in arch height is explained by genetics.
- Genome-wide association studies (GWAS) have linked variants in cartilage-related genes (including COMP, COL9A1, and GDF5) to osteoarthritis susceptibility across multiple joints, including the foot.
- The AOFAS notes that hallux rigidus without a prior injury history has strong hereditary patterns, especially in bilateral cases (both feet affected).
Does Family History Mean You Will Definitely Develop Hallux Rigidus?
Not necessarily. Having genetic risk factors increases your probability, but does not guarantee you will develop the condition. The relationship between hallux rigidus genetics and disease expression is what scientists call polygenic and multifactorial; multiple genes interact with environmental triggers to determine outcomes. This means proactive prevention strategies can meaningfully reduce risk even with genetic predisposition.
The importance of early detection ranks as a top priority for genetically predisposed individuals. Early-stage hallux rigidus (Grade 1) responds well to conservative care, including custom orthotics, footwear modifications, and physical therapy — all of which can significantly slow progression.
Practical Steps If Hallux Rigidus Runs in Your Family
If you have a family history of hallux rigidus, taking these proactive steps can help delay or minimize the impact of the condition:
- Get a baseline assessment from a podiatrist before symptoms appear. Weight-bearing X-rays can identify structural risk factors early. See our guide on X-rays and MRIs in early detection.
- Choose supportive footwear. Avoid flat, unsupportive shoes that worsen pronation. Our guide to the best shoes for hallux rigidus covers options by severity level.
- Use custom orthotics if you have flat feet or first ray hypermobility. A podiatrist can prescribe orthotics that correct biomechanical abnormalities.
- Maintain a healthy weight. Every kilogram of body weight adds approximately 3 kilograms of force on the forefoot during walking. Weight management reduces cumulative joint stress.
- Monitor for early signs. Morning stiffness, difficulty bending the big toe upward, and pain after activity are early warning signs. Learn the early signs of hallux rigidus so you can act before damage advances.
- Know when to see a doctor. If you notice any of these symptoms, check our guide on when to see a doctor for toe pain.
Frequently Asked Questions About Hallux Rigidus Genetics
Is hallux rigidus hereditary?
Yes, hallux rigidus has a strong hereditary component. Studies show that up to 80% of patients have a positive family history of foot problems. The inherited traits most linked to hallux rigidus include flat feet, elevated first metatarsal, first ray hypermobility, and square metatarsal head morphology.
Can hallux rigidus genetics be tested?
There is currently no specific genetic test for hallux rigidus. However, structural risk factors (flat feet, elevated first metatarsal, etc.) can be identified through weight-bearing X-rays and physical examination. If you have a family history, asking your podiatrist to assess these structural factors is the most actionable approach available today.
Does having a parent with hallux rigidus mean I will get it?
Having an affected parent increases your risk, but it does not guarantee you will develop the condition. Gene expression depends on multiple factors, including activity level, footwear choices, body weight, and whether you sustain traumatic injuries to the joint. Proactive foot care can significantly offset inherited risk.
Is bilateral hallux rigidus more genetic?
Yes. Bilateral cases (both feet affected) are more strongly associated with hereditary risk factors than unilateral cases. When both feet develop hallux rigidus without a history of single-limb trauma, clinicians consider genetics the primary driver.
Can genetic hallux rigidus be prevented?
While you cannot change your genetic predisposition, proactive interventions can slow how the condition progresses. Appropriate footwear, custom orthotics, weight management, and regular podiatric monitoring can delay onset and slow progression even in genetically predisposed individuals.
Medically Reviewed: The editorial team at HalluxRigidusCare.com reviewed this article for clinical accuracy. All references are sourced from peer-reviewed literature and professional medical organizations including AOFAS, NCBI/PubMed, and the Journal of Bone and Joint Surgery.