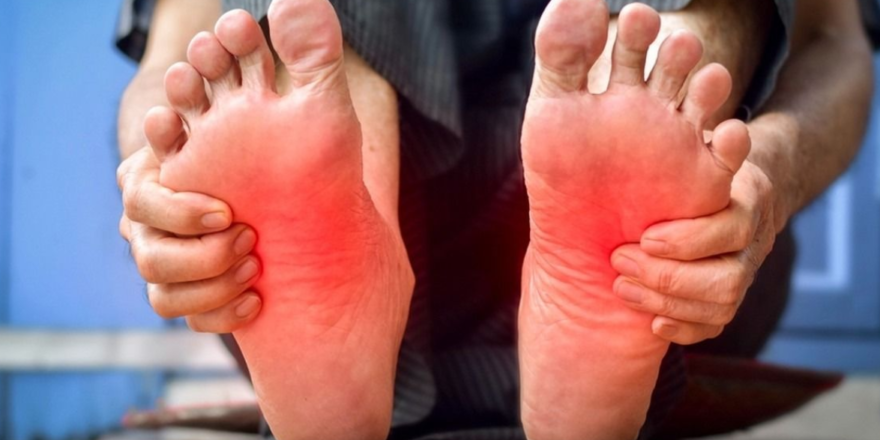
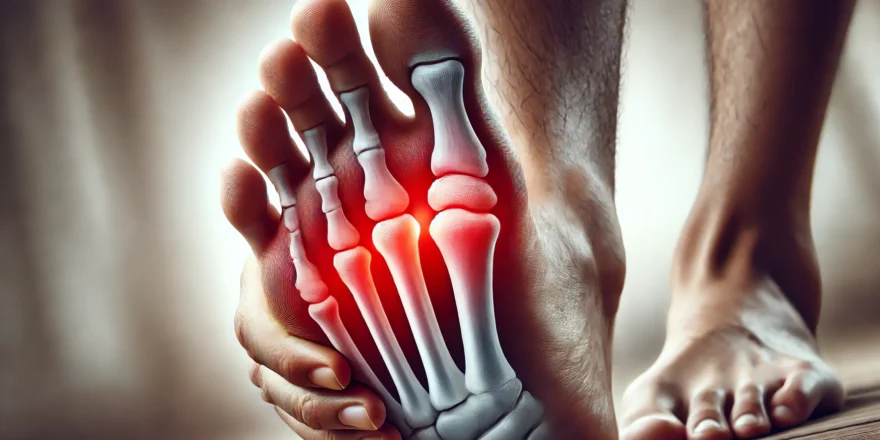
Are your toes showing signs they’ve lost their spark? Knowing when to see a doctor for toe pain can feel overwhelming, especially when the discomfort comes and goes. Toe pain has an uncanny way of sneaking up on you like a silent thief in the night. One moment you’re walking through the park, and next, a sharp “locking” sensation stops you in your tracks.
📋 In This Guide
- 7 specific red flags that mean you should see a podiatrist this week
- Symptoms that can wait vs. those requiring urgent evaluation
- What to expect at your first podiatry appointment for toe pain
- Questions to ask your doctor to get the most from your visit
If this discomfort centers around your big toe joint, Hallux Rigidus may be the silent culprit. Recognizing the signs of when to see a doctor for toe pain early can be the difference between a simple shoe change and a surgical procedure.
This guide walks you through every clinical red flag you cannot afford to ignore, including a self-test you can do at home right now.
What Is Hallux Rigidus? (The Engine Under Your Foot)
To understand why you need help, you must first understand what’s breaking down.
The big toe, technically called the Hallux, is the most important mechanical lever in your entire body. In fact, every step you take depends on it bending properly. When it becomes Rigidus (stiff), that lever stops working.
Hallux Rigidus is a form of degenerative arthritis that specifically targets the metatarsophalangeal (MTP) joint, the large knuckle at the base of your big toe. The slippery cartilage cushion between the bones slowly erodes, leading to bone-on-bone friction. Your body attempts to protect itself by growing osteophytes (bone spurs), which eventually create a mechanical block that makes bending your toe feel like trying to flex a rusted steel rod.
According to the American Academy of Orthopaedic Surgeons, hallux rigidus is the most common arthritic condition of the foot, affecting 1 in 40 people over the age of 50.
______________________________________________________________________________________________________________________________________
The 4 Stages of a Stiff Toe: Where Are You Right Now?
Understanding your stage is the first step in deciding when to see a doctor for toe pain.
- Stage 1 — Hallux Limitus (Early Warning): Mild tightness only at the end of a bend. You may notice stiffness after sitting for long periods or during hill walking. Pain is minimal.
- Stage 2 — Moderate Progression: Visible bone spurs begin forming on top of the joint. Flexibility is reduced by up to 50%. You may start unconsciously limping or shifting your weight to avoid bending the toe.
- Stage 3 — Advanced Hallux Rigidus: Constant pain during walking with noticeable gait changes. The bump on top of the toe becomes visible and painful against the shoe uppers. Daily activity is significantly affected.
- Stage 4 — End-Stage (Fused Joint) The joint is essentially non-functional. At this stage, surgery is usually your only effective option
The critical window is Stages 1–2. Conservative treatment (rigid-sole shoes, custom orthotics) works best here. By Stage 3–4, your options narrow significantly.
5 Red Flags: When to See a Doctor for Toe Pain
Pain is your body whispering. If you ignore the whispers, your body will eventually shout. These red flags tell you when to see a doctor for toe pain is no longer optional.

🚩 Red Flag #1 — The 72-Hour Pain Rule
If sharp pain or a “locking” sensation in your big toe joint persists for more than 72 hours despite rest, ice, and elevation, this is a structural signal, not a passing strain. Active joint inflammation can rapidly accelerate cartilage loss. Professional diagnosis at this point is essential.
🚩 Red Flag #2 — The “Windlass” Gait Compensation
Stand up and walk right now. Are you unconsciously tilting your weight to the outer edge of your foot? This is called supination, your body’s way of protecting the painful toe by avoiding it altogether.
While it saves your toe in the short term, consequently, this compensation pattern causes secondary pain in your knees, hips, and lower back within months. If you notice this shift in how you walk, you are already in Stage 2 or beyond.
🚩 Red Flag #3 — The Dorsal Bump
Unlike a regular bunion (which grows on the side of the toe), Hallux Rigidus creates a “Dorsal Bunion“, a hard, bony ridge on the TOP of the joint. Run your finger across the top of your big toe knuckle. If you feel a firm, raised lump that makes shoe-wearing uncomfortable, you are seeing physical evidence of bone spurs. This needs imaging to assess the extent of damage.
🚩 Red Flag #4 — Pain at Rest or at Night
Early Hallux Rigidus hurts during activity and eases at rest. If you begin experiencing pain while sitting, lying down, or at night, this indicates significant joint inflammation and a more advanced stage. This is also a key differentiator from gout (see the comparison table below).
🚩 Red Flag #5 — Shoe Modifications Are No Longer Working
If you’ve already switched to wider shoes or softer soles and your pain is still worsening, conservative self-management has reached its limit. A podiatrist needs to assess whether you need custom orthotics, corticosteroid injections, or surgical evaluation.
The Home Self-Test: When Toe Pain Needs Attention
Mark’s Pro-Tip — The Hand Test: Sit down and place your foot flat in front of you. Use your hand to gently pull your big toe upward toward your shin. A healthy MTP joint should allow at least 50–60 degrees of upward movement with mild resistance.
If you cannot reach 50 degrees, or if you feel a sharp, stabbing sensation before reaching that range, your joint mobility is already compromised. Book a podiatry appointment this week, not next month.
______________________________________________________________________________________________________________________________________
Hallux Rigidus vs Gout vs Bunion: Know the Difference
One of the most common questions we receive is how to distinguish between these three conditions. They all affect the big toe, but they are entirely different problems requiring different treatment.
Feature | Hallux Rigidus | Gout | Bunion |
Onset | Gradual, over months/years | Suddenly, often overnight | Gradual |
Pain Type | Mechanical stiffness | Intense burning/throbbing | Pressure & aching |
Redness/Heat | Mild | Severe, dramatic | Mild |
Location | Top of joint (dorsal) | Entire toe, very diffuse | Side of joint (medial) |
Pain at Rest | Only in advanced stages | Yes, extremely painful | Occasional |
Trigger | Movement, activity | Rich food, alcohol, dehydration | Narrow shoes |
Best Test | Range of motion test | Blood uric acid test | Visual/X-ray |
Bottom line: If your toe flared up overnight with extreme redness and heat, see a doctor today; that’s likely gout. If it’s been gradually stiffening over months, it’s likely Hallux Rigidus.
Red Flags by Age Group
The condition behaves differently depending on your age, and so does the urgency to act.

- Under 40: Hallux Rigidus at a younger age is often linked to a previous injury, Morton’s Toe (long first metatarsal), or repetitive athletic stress. At this age, joint-sparing surgery (cheilectomy) is highly effective and worth pursuing early. Don’t wait.
- 40–60 Years Old: This is the peak window for onset. Conservative treatment works well if caught in Stages 1–2. Rigid-sole footwear and custom orthotics can manage symptoms for years. See a podiatrist within 2–4 weeks of noticing red flags.
- 60 and Over: Cartilage naturally thins with age, accelerating progression. If you are in Stage 3–4, joint fusion (arthrodesis) becomes the most reliable long-term solution.
The good news: most patients return to normal activity after fusion, including walking and light jogging. What Happens If You Wait Too Long?
Delaying a podiatry visit doesn’t just mean more pain; it means fewer options.
- Stage 1 untreated → Stage 2: Subsequently, bone spurs form and cannot be reversed without surgery
- Stage 2 untreated → Stage 3: Gait compensation begins, causing knee and hip pain
- Stage 3 untreated → Stage 4: The joint essentially fuses on its own, but painfully and in the wrong position
- End-stage without treatment: Your surgeon will likely recommend joint fusion only, which permanently eliminates toe movement
The difference between a $40 pair of rigid-sole insoles and an $8,000 surgical procedure often comes down to how quickly you acted.

______________________________________________________________________________________________________________________________________
Why Does Hallux Rigidus Develop? (The Real Causes)
However, Hallux Rigidus rarely appears from nowhere. The most common contributors include:
- Repetitive Stress: Runners, hikers, and people who stand for long hours wear down the MTP joint cartilage over time. This is why athletes in their 30s and 40s are disproportionately affected.
- Genetic Predisposition: Having a “Long First Metatarsal” or “Morton’s Toe” places excess mechanical leverage on the MTP joint with every step.
- Previous Injury: A single severe turf toe injury or repeated minor sprains can damage the cartilage, triggering early arthritis.
- Inflammatory Conditions: Rheumatoid arthritis, gout, and psoriatic arthritis can all accelerate cartilage erosion in the MTP joint.
What to Expect at Your Podiatrist Appointment
In 2026, modern podiatry focuses on Joint Preservation, saving the joint rather than replacing or fusing it whenever possible.
Here’s exactly what will happen:
- Step 1 — Mechanical Examination: The podiatrist will physically test your range of motion and feel for a “hard stop” in the joint — the point where bone is blocking bone rather than cartilage cushioning movement.
- Step 2 — Weight-Bearing X-Rays: Unlike a standard X-ray taken lying down, weight-bearing X-rays show exactly how much joint space remains when your full body weight is applied. This is the gold standard for accurately staging Hallux Rigidus.
- Step 3 — Treatment Planning: Based on your stage, they will recommend a conservative management plan (orthotics, rigid-sole shoes, NSAIDs, injections) or discuss surgical options if you are Stage 3–4.
Treatment Pathways: Reclaiming Your Stride
Conservative Care (Stages 1–2):
- Rigid-sole shoes with rocker bottoms
- Carbon fiber Morton’s extension insoles
- Custom orthotic devices
- NSAIDs for inflammation management
- Corticosteroid injections for flare-ups
Switching to properly designed footwear is often the single most impactful first step. See our guide to the best shoes for hallux rigidus for podiatrist-recommended options at every budget.
Surgical Options (Stages 3–4):
- Cheilectomy — bone spur removal, preserves joint motion. Best results in Stages 1–2
- Interpositional Arthroplasty — removes damaged bone and inserts a spacer
- Arthrodesis (Joint Fusion) — permanent pain relief, limits toe movement. Gold standard for advanced stages
The Podiatrist Appointment Checklist
Screenshot this and bring it to your appointment:
- “What stage is my Hallux Rigidus currently in?”
- “Do my X-rays show joint space narrowing or just bone spurs?”
- “Am I a candidate for a joint-sparing procedure like a cheilectomy?”
- “What specific rigidity grade should I look for in footwear?”
- “Should I consider custom orthotics or are over-the-counter carbon fiber insoles sufficient?”
- “How quickly is my condition likely to progress without intervention?”
Conclusion: When to See a Doctor for Toe Pain — Act Now!
Recognizing when to see a doctor for toe pain is the most proactive thing you can do for your long-term mobility. Furthermore, the window between manageable and surgical is real, and it closes faster than most people expect.
If you identified even one red flag in this guide, the next step is clear: book a podiatry appointment this week.
Once diagnosed, your podiatrist will almost certainly recommend rigid-sole footwear as part of your management plan. When that time comes, see our guide to the best walking shoes for hallux rigidus reviewed and rated specifically for each stage of the condition.
______________________________________________________________________________________________________________________________________
Frequently Asked Questions About When to See a Doctor for Hallux Rigidus
Can Hallux Rigidus be reversed without surgery?
The physical bone spurs cannot be dissolved, but symptoms can be effectively managed, and progression slowed significantly. Rigid-sole shoes and custom orthotics offload the joint and stop the bone-on-bone friction that drives pain and deterioration.
Is it okay to walk with a stiff big toe?
Yes — but only in appropriate footwear. Flexible, “bendy” shoes force the arthritic joint to bend with every step, increasing inflammation and accelerating damage. Rocker-bottom or rigid-soled shoes allow you to stay active without aggravating the joint.
How do I tell the difference between Hallux Rigidus and Gout?
Gout typically appears suddenly (often overnight) with intense redness, heat, and extreme sensitivity to even light touch. Hallux Rigidus is a gradual mechanical stiffness that worsens with activity and eases at rest — at least in the early stages.
Will wearing wide-toe-box shoes help?
Absolutely. A wide toe box reduces pressure on the dorsal bone spur, preventing the skin irritation and bursitis that often accompany an arthritic joint. Pair a wide toe box with a rigid or rocker sole for maximum relief.
What is the best self-test for big toe pain I can do at home?
Use the Hand Test described above. If you cannot pull your big toe upward to 50 degrees without sharp pain, your range of motion is clinically compromised. This is a reliable early indicator that warrants a professional evaluation.
How long can I manage Hallux Rigidus without surgery?
Many patients manage Stage 1–2 conservatively for 5–10+ years with the right footwear and orthotics. However, if conservative measures stop working or your stage advances to 3–4, surgical evaluation becomes necessary.
You experience any of the following: toe pain that persists beyond 2 weeks despite rest, visible deformity or hard bony bump on the joint, pain that changes how you walk, or swelling that does not improve with ice and elevation. Early-stage hallux rigidus (Grade 1–2) responds well to conservative care — waiting too long limits your treatment options.
>
- When to See a Doctor for Toe Pain: The Ultimate Hallux Rigidus Red Flag Guide (2026) - March 11, 2026
- Early Signs of Hallux Rigidus: Key Symptoms & Prevention - November 5, 2025
- The Role of X-Rays and MRIs in Detecting Hallux Rigidus Early - April 21, 2025