In This Guide
- What Hallux Rigidus is and how it progresses over time
- The 4 clinical stages are explained in plain language
- How HR differs from bunions, gout, and turf toe
- Your full treatment roadmap — from conservative care to surgery
Hallux rigidus is a degenerative arthritis of the first metatarsophalangeal (MTP) joint. The knuckle at the base of the big toe causes progressive stiffness, pain, and loss of upward (dorsiflexion) movement. It is the most common form of arthritis in the foot and the leading cause of big toe joint pain in adults over 30.
What You’ll Learn
- What is hallux rigidus — degenerative arthritis of the big toe joint (MTP joint)
- The 4 severity grades — from mild stiffness to complete joint space loss
- Key symptoms — pain, swelling, bone spurs, restricted dorsiflexion
- Treatment options — from footwear changes to surgery, matched to the grade
Unlike a bunion, which causes lateral deviation of the big toe, hallux rigidus primarily affects joint mobility. As cartilage erodes, bone spurs (osteophytes) form on the top of the joint, mechanically blocking the upward movement needed for walking, running, and climbing stairs. Understanding this condition is the first step to managing it effectively.
What Is Hallux Rigidus? Definition and Anatomy
The term “hallux rigidus” comes from Latin: hallux means big toe, and rigidus means stiff. The condition affects the first MTP joint, where the first metatarsal bone of the foot meets the proximal phalanx of the big toe. This joint bears approximately 50–60% of body weight during the push-off phase of walking, making it highly susceptible to repetitive stress and cartilage breakdown.
In a healthy joint, smooth hyaline cartilage allows frictionless movement. In hallux rigidus, this cartilage degenerates, causing bone-on-bone contact. The body responds by growing bone spurs, which progressively restrict the 50–70° of dorsiflexion normally required for normal gait.
According to the American Orthopaedic Foot & Ankle Society (AOFAS), hallux rigidus affects approximately 1 in 40 adults over the age of 50.
Root Causes and Risk Factors
The exact causes of hallux rigidus remain an active area of research, but several well-established risk factors contribute to its development:
- Structural abnormalities: A long first metatarsal, flat feet, or a square metatarsal head increase joint stress and predispose individuals to early cartilage wear
- Genetics: Family history plays a major role. Studies show that up to 80% of patients have a close relative with foot problems
- Prior joint injury: A single traumatic event, such as a turf toe injury or repetitive microtrauma from sports, can trigger cartilage degeneration
- Inflammatory conditions: Rheumatoid arthritis, gout, and psoriatic arthritis can accelerate joint damage
- Footwear history: Prolonged use of narrow, rigid, or high-heeled shoes increases MTP joint stress over time
Research published on PubMed/NCBI by Coughlin and Shurnas (2003) remains the landmark study on hallux rigidus. Classifying 110 cases and confirming the strong hereditary component, particularly through inherited foot structure.
Hallux Rigidus Symptoms: What to Expect
Hallux rigidus symptoms typically develop gradually and worsen over time without treatment. The most common signs include:
- Pain and stiffness at the big toe joint, worsened by activity and relieved by rest
- Swelling around the MTP joint, particularly after prolonged walking or standing
- A visible bump on top of the joint — bone spurs that can be felt and seen
- Difficulty wearing shoes due to the dorsal prominence and limited range of motion
- Changes in gait: patients naturally begin walking on the outer edge of the foot to avoid painful push-off, causing secondary knee, hip, and lower back strain
- Dull ache at rest in advanced stages, indicating significant joint damage
Grading is critical for treatment decisions. Grades 1–2 respond well to conservative management (orthotics, footwear, injections). Grade 3 often benefits from cheilectomy (bone spur removal). Grade 4 typically requires arthrodesis (joint fusion) — permanent but highly effective for eliminating pain.
Staging the Condition: From Mild to Severe
Hallux rigidus is classified into four grades based on clinical and radiological findings. The Coughlin-Shurnas grading system is the most widely used:
| Grade | Dorsiflexion | X-ray Findings | Symptoms | Treatment |
|---|---|---|---|---|
| Grade 1 | 20–50° | Mild osteophytes | Mild stiffness, pain at extremes of motion | Supportive footwear, orthotics |
| Grade 2 | 10–20° | Moderate osteophytes, joint space narrowing | Moderate pain, limited activity | Stiff-soled shoes, NSAIDs, injections |
| Grade 3 | <10° | Significant osteophytes, marked joint space loss | Severe pain, significantly restricted daily activities | Cheilectomy surgery |
| Grade 4 | ~0° | Complete joint space loss, subchondral cysts | Constant pain even at rest | Arthrodesis (joint fusion) |
Treatment Options for Hallux Rigidus
Treatment depends on grade severity. For Grades 1–2, conservative management is effective in the majority of patients:
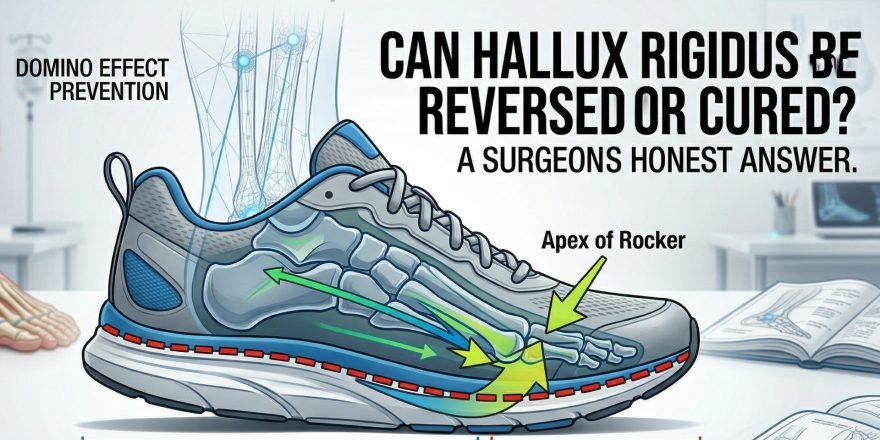
- Footwear modifications: Stiff-soled shoes with a rocker bottom reduce MTP joint dorsiflexion demand — the foundation of non-surgical treatment
- Custom orthotics: A Morton’s extension insole blocks painful joint motion without restricting the shoe
- NSAIDs: Ibuprofen or naproxen reduce inflammation and pain in the short term
- Corticosteroid injections: Provide relief for 3–6 months in moderate cases
- Physical therapy: Joint mobilization and strengthening of the intrinsic foot muscles can slow progression
For Grade 3, cheilectomy, the surgical removal of bone spurs, restores motion with excellent long-term outcomes. Grade 4 typically requires arthrodesis (joint fusion), which eliminates pain at the cost of permanent motion loss. Learn more in our guide on Hallux Rigidus Causes, Symptoms and Treatment.
Further Reading and Expert Resources
Now that you understand what hallux rigidus is, explore these in-depth resources to manage and treat the condition effectively:
- Hallux Rigidus Causes, Symptoms & Treatment Options — complete clinical breakdown
- Early Signs of Hallux Rigidus — catch it before it progresses to Grade 3+
- Best Shoes for Hallux Rigidus — the most evidence-based footwear guide online
- Hallux Rigidus vs. Bunions, Gout & Turf Toe — accurate diagnosis matters
- Why Early Detection of Hallux Rigidus Matters — how to prevent Grade 3+ progression
Frequently Asked Questions
Is hallux rigidus the same as arthritis?
Yes — hallux rigidus is a form of osteoarthritis specifically affecting the first MTP joint of the big toe. It involves the same cartilage degeneration and bone spur formation seen in other arthritic joints.
Can hallux rigidus be reversed?
Cartilage loss cannot be reversed, but symptoms can be effectively managed with conservative treatment in Grades 1–2. Early intervention significantly slows progression and can preserve function for decades.
Does hallux rigidus always require surgery?
No. The majority of Grade 1–2 cases respond well to conservative management, including appropriate footwear, orthotics, and physical therapy. Surgery is typically reserved for Grade 3–4 cases where conservative care has failed.
What is the difference between hallux rigidus and hallux valgus?
Hallux valgus (bunion) involves lateral deviation of the big toe caused by a widening of the forefoot angle. Hallux rigidus involves stiffness and arthritis of the big toe joint without significant deviation. The two conditions can coexist.
How quickly does hallux rigidus progress?
Progression varies widely. Some patients remain at Grade 1–2 for decades with good footwear management; others progress from Grade 1 to Grade 3 within 5–7 years without intervention. Early detection and treatment are the most effective predictors of outcome.
Medically Reviewed: This article was reviewed for clinical accuracy by the editorial team at HalluxRigidusCare.com. All references are sourced from peer-reviewed literature and professional medical organizations, including AOFAS, NCBI/PubMed, and the Journal of Bone and Joint Surgery.
- Hallux Rigidus Myths Debunked: What Athletes Need to Know - January 14, 2025
- What Is Hallux Rigidus? Complete Guide to Causes, Symptoms & Treatment - October 16, 2023