Accurate hallux rigidus diagnosis is the first step toward effective treatment. Hallux rigidus, a form of degenerative arthritis affecting the big toe’s metatarsophalangeal (MTP) joint, is frequently misidentified as a bunion, gout, turf toe, or sesamoiditis.
Each of these conditions requires a different treatment approach, making proper diagnosis critical. In this comprehensive clinical guide, you will learn exactly how to distinguish hallux rigidus from other toe conditions using symptom profiles, physical examination findings, and diagnostic imaging.
📋 What This Guide Covers
- 5 conditions commonly confused with hallux rigidus — and how to tell them apart
- Key diagnostic differences in location, movement, and X-ray findings
- Why correct diagnosis matters — each condition requires a different treatment approach
- Red flags that indicate you need imaging to confirm the diagnosis
What Is Hallux Rigidus? A Clinical Overview
Hallux rigidus is the most common arthritic condition of the foot, affecting an estimated 2.5% of adults over age 50 according to research published by the National Institutes of Health (NIH).
The condition develops as cartilage in the first MTP joint breaks down over time, leading to bone-on-bone contact, bone spur formation, and progressive loss of motion, particularly dorsiflexion (bending the toe upward). For a complete overview of this condition, see our guide to what is hallux rigidus.
Common Symptoms to Watch For
- Pain and stiffness in the big toe joint, especially during push-off activities
- Reduced dorsiflexion — difficulty bending the toe upward beyond 20 to 30 degrees
- A dorsal bone spur forms on the top of the joint, visible or palpable
- Swelling and inflammation around the first MTP joint after activity
- Altered gait — walking on the outer edge of the foot to avoid toe bend
- Worsening pain in cold or damp weather — a classic arthritic symptom
Hallux Rigidus Diagnosis vs. Other Toe Conditions: Side-by-Side Comparison
One of the most important steps in hallux rigidus diagnosis is ruling out conditions with similar presentations. The table below compares hallux rigidus against the five most commonly confused toe conditions.
| Condition | Location | Key Symptom | Onset | Confirmed By |
|---|---|---|---|---|
| Hallux Rigidus | 1st MTP joint (top) | Stiff toe, dorsal spur, limited dorsiflexion | Gradual (degenerative) | X-ray: joint space narrowing, osteophytes |
| Bunion (Hallux Valgus) | 1st MTP joint (medial side) | Lateral deviation of big toe, medial bump | Gradual | X-ray: hallux valgus angle above 15 degrees |
| Gout | 1st MTP joint (podagra) | Sudden severe pain, red hot swollen joint | Acute flare (hours) | Blood: elevated uric acid; joint fluid analysis |
| Turf Toe | 1st MTP joint (plantar) | Pain on plantar side after hyperextension injury | Acute (traumatic) | MRI: plantar plate or capsule tear |
| Sesamoiditis | Under 1st MTP (sesamoid bones) | Pain under big toe, worsens with toe pressure | Gradual or acute | X-ray or bone scan: sesamoid inflammation |
| Hallux Limitus | 1st MTP joint | Reduced motion 20 to 50 degrees, early-stage stiffness | Gradual (early arthritis) | Physical exam plus X-ray: mild joint changes |
Hallux Rigidus vs. Bunion: Key Differences
Bunions (hallux valgus) and hallux rigidus are both conditions of the first MTP joint, but differ fundamentally in mechanics and appearance. A bunion causes the big toe to deviate laterally toward the second toe, creating a prominent medial bony protrusion at the base of the big toe. Pain is typically felt along the inner edge of the joint, especially from shoe pressure.
In contrast, hallux rigidus diagnosis is indicated when the bony prominence sits on top of the joint rather than the side, and the dominant complaint is stiffness and limited upward motion. The toes may remain straight. A patient can have both conditions simultaneously, which is why imaging is essential.
Research confirms that the hallux valgus angle on weight-bearing X-ray confirms bunion diagnosis, while dorsal osteophytes and joint space narrowing confirm hallux rigidus.
Hallux Rigidus vs. Gout: Telling Them Apart
Gout is a metabolic condition caused by uric acid crystal deposition in joints. It most commonly affects the first MTP joint, the same joint as hallux rigidus. Misdiagnosis is common and clinically significant because gout requires systemic urate-lowering therapy, while hallux rigidus is managed mechanically and surgically.
Key differentiating features: Gout attacks are sudden, typically occurring at night, with the joint becoming intensely red, hot, and exquisitely tender within hours. Hallux rigidus pain develops gradually over months to years, worsens with specific movements (dorsiflexion), and lacks the systemic inflammatory response seen in gout.
Blood work showing elevated serum uric acid and synovial fluid analysis confirming monosodium urate crystals confirms gout. Consult a podiatrist or rheumatologist for proper hallux rigidus diagnosis and differential workup. You can also learn about common risk factors that make some people more susceptible.
Traumatic Turf Toe vs. Degenerative Arthritis
Turf toe is a sports injury involving sprain or tear of the plantar plate and joint capsule of the first MTP joint, typically caused by hyperextension. Common in football players and athletes on artificial turf, turf toe pain is concentrated on the bottom (plantar) surface of the joint and follows a clear traumatic event.
Hallux rigidus develops insidiously over the years without a single injury event. Pain in hallux rigidus is typically dorsal, aggravated by toe bend during push-off. An MRI is the gold standard for diagnosing turf toe, while hallux rigidus diagnosis relies primarily on weight-bearing X-rays. Athletes who sustain turf toe injuries may be at increased risk of developing hallux rigidus later, as joint damage accelerates degenerative changes.
See our complete guide on early signs of hallux rigidus to catch this before it worsens.
How Is Hallux Rigidus Diagnosed? A Clinical Step-by-Step Approach
Step 1: Physical Examination and Range of Motion
A podiatrist or orthopedic surgeon will assess the range of motion at the first MTP joint. Normal dorsiflexion is approximately 60 to 70 degrees. In hallux rigidus, dorsiflexion is typically less than 30 degrees (Grade 2) or absent (Grades 3 and 4). The grind test, passively rotating the joint while applying axial load, reproduces pain and indicates cartilage damage.
Step 2: Weight-Bearing X-Rays
Weight-bearing radiographs are the cornerstone of hallux rigidus diagnosis. Signs include: joint space narrowing, dorsal osteophytes, subchondral sclerosis, and flattening of the metatarsal head. The Coughlin-Shurnas grading system (Grades 0 to 4) classifies severity based on X-ray findings and clinical symptoms. Learn more about how X-rays and MRIs detect this condition early.
Step 3: Advanced Imaging When Needed
MRI is reserved for cases where soft tissue pathology needs assessment. CT scans help in surgical planning for advanced cases. Blood work (uric acid, ESR, CRP, rheumatoid factor) rules out metabolic or autoimmune causes.
Treatment Options for Each Hallux Rigidus Grade
According to the American Orthopaedic Foot and Ankle Society (AOFAS), treatment is graded by severity:
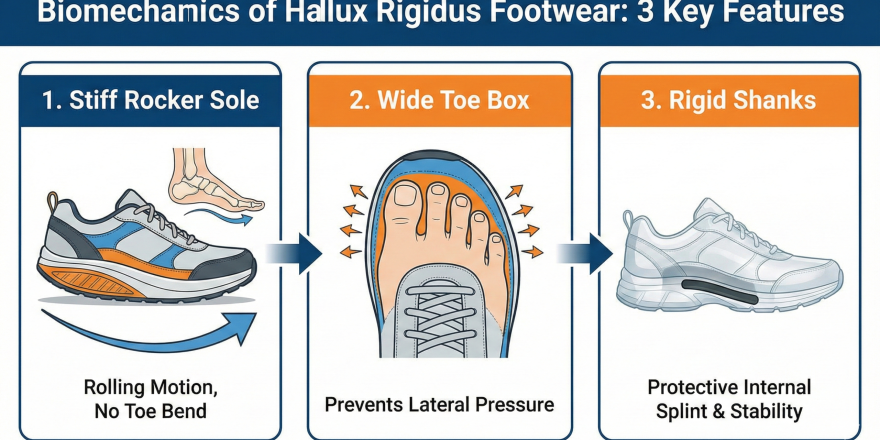
- Grade 1 (Mild): Stiff-soled shoes, physical therapy, NSAIDs, cortisone injections
- Grade 2 (Moderate): Custom orthotics, stiff rocker-bottom shoes, activity modification
- Grade 3 (Severe): Cheilectomy (surgical bone spur removal) is often recommended
- Grade 4 (End-stage): Arthrodesis (joint fusion) or total joint replacement
The earlier a correct hallux rigidus diagnosis is made, the greater the likelihood of avoiding surgery. Read about the importance of early detection and intervention for best outcomes. For a complete look at all treatment options, see our guide on hallux rigidus causes, symptoms and treatment.
Hallux rigidus is often misdiagnosed as gout or a bunion. The key distinguishing feature is restricted dorsiflexion (upward movement) of the big toe. If your toe is stiff moving upward but mobile side-to-side, hallux rigidus is the most likely cause. Gout presents with redness and warmth; bunions show lateral deviation without primary stiffness.
Frequently Asked Questions About Hallux Rigidus Diagnosis
Can This Condition Be Mistaken for a Bunion?
Yes, this is one of the most common misdiagnoses. Both conditions affect the first MTP joint, but a bunion involves lateral toe deviation with a medial bump, while hallux rigidus causes joint stiffness with a dorsal bone spur and no lateral deviation. X-rays clearly distinguish the two.
What Does It Feel Like Compared to Gout?
Hallux rigidus pain is chronic and mechanical, worsening with toe movement over months or years. Gout pain is acute and inflammatory; the joint becomes suddenly red, hot, and intensely painful, often overnight, without a preceding injury or activity change.
Is It Visible on an X-ray?
Yes. Weight-bearing X-rays typically show joint space narrowing, bone spur formation on the dorsal aspect, and sclerosis of the joint surfaces. These findings are sufficient for a clinical hallux rigidus diagnosis in most cases.
Can I Self-Diagnose at Home?
You can identify warning signs at home: try bending your big toe upward. If you experience pain or stiffness and can barely lift it beyond 20 degrees, that is a red flag. However, confirmation requires X-rays and physical examination by a qualified podiatrist or orthopedic surgeon. Learn about when to see a doctor for toe pain.
Which Specialist Should You See?
A podiatrist (foot and ankle specialist) or an orthopedic surgeon with foot and ankle subspecialty training is the most qualified clinician for hallux rigidus diagnosis. Rheumatologists may also be involved if autoimmune or metabolic causes need to be ruled out.
How Does This Condition Progress Over Time?
Without treatment, hallux rigidus typically progresses through four grades: from mild stiffness and occasional pain (Grade 1) to complete joint ankylosis with no motion (Grade 4). Early intervention significantly slows progression. See our article on the role of genetics in hallux rigidus development for more on why some people progress faster than others.
Medically Reviewed: This article was reviewed for medical accuracy by the editorial team at HalluxRigidusCare.com. All clinical references are sourced from peer-reviewed literature and professional medical organizations, including AOFAS and NIH.